News All News
February 8th, 2019
Toward safer bone-marrow transplants
New advances selectively suppress damaged cells, allowing for transplants without chemotherapy or radiation
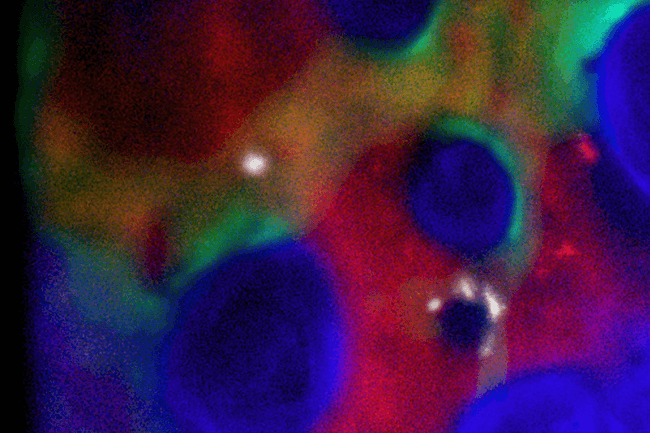
Pictured are hematopoietic stem cells (white) as they find their niche in the bone marrow after transplantation. (Image courtesy of the research team.)
Blood stem cell transplants — also known as bone-marrow transplants — can cure many blood, immune, autoimmune, and metabolic disorders, from leukemia to sickle-cell disease. But to make sure the healthy blood cells “take,” doctors first have to deplete the patient’s own, defective blood stem cells using intensive chemotherapy or whole-body radiation. This wipes out the patient’s immune system, raising the risk of infection and often causing serious side effects, including anemia, infertility, secondary cancers, organ damage, and even death.
“We know that stem cell transplants can cure dozens of blood disorders, including exciting progress with treating autoimmunity,” said Professor David Scadden, co-director of the Harvard Stem Cell Institute and director of the Center for Regenerative Medicine at Massachusetts General Hospital. “Yet they are rarely used beyond treating blood cancers because of the extreme rigors the patients must endure.”
New research led by Scadden and his colleagues at Harvard University has demonstrated in mice an effective alternative to this toxic pretreatment. Published in Nature Communications, the findings pave the way for clinical studies that will show whether the method would work in humans, making blood stem cell transplants safer and available to more patients.
“If the principles demonstrated in these studies translate to the clinic, they open the possibility of expanding stem cell transplantation to many more patients who we know would benefit if only it were made more tolerable,” said Derrick Rossi, co-senior author of the paper.
The innovations were enabled in part by OTD's Blavatnik Biomedical Accelerator, and have been licensed to Magenta Therapeutics. Read more in the Harvard Gazette.
Tags: accelerator , stem cells , Blavatnik Biomedical Accelerator
Press Contact: Kirsten Mabry | (617) 495-4157
